🧠 The Case
A 5-month-old infant presents to the ED with:
- 1 day of diffuse cyanosis
- Slight irritability
- No respiratory distress
- Capillary refill: 3–4 seconds
Initial Workup:
- pH: 7.49
- CO₂: 29
- SpO₂: low—but improving only slightly with supplemental oxygen
- And one more thing:
“The blood drawn looked… brownish.”
🩸 The Turn: Chocolate Blood + Unexpected Hypoxia
Blood gas reveals a methemoglobin level of 31.6%
(normal is <1.5%)
You immediately recognize this as methemoglobinemia—a condition where hemoglobin is oxidized (Fe²⁺ ➝ Fe³⁺) and can no longer carry oxygen effectively. Even supplemental O₂ won’t help, because the hemoglobin is functionally useless at transport.
🔍 Diagnosis Clues
- Cyanosis without significant respiratory distress
- Pulse oximetry that doesn’t match the patient’s appearance or gas
- Chocolate-colored blood that doesn’t turn red on exposure to air
- History of diarrhea, possible nitrate exposure, or idiopathic onset in infants under 6 months
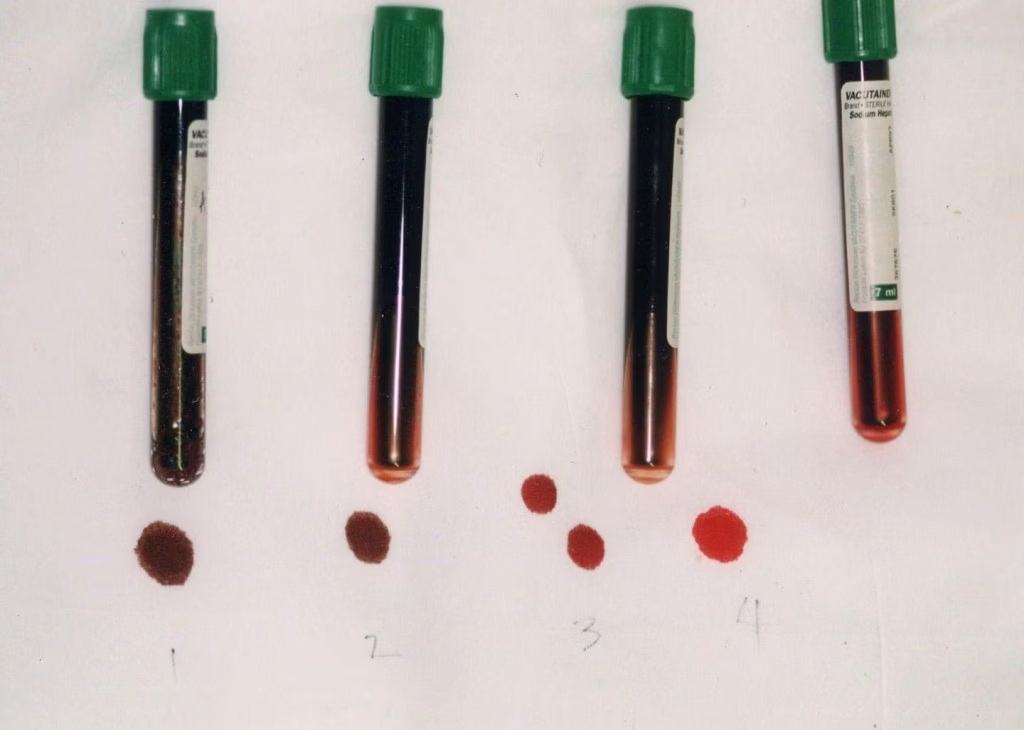
Chocolate brown color of methemoglobinemia: In tubes 1 and 2, methemoglobin fraction is 70%; in tube 3, 20%; and in tube 4, normal. (Source: Medscape)
💊 Management
- If asymptomatic and MetHb < 20% → Supportive care
- If symptomatic or MetHb > 30% →
Methylene Blue is the treatment of choice
(1–2 mg/kg IV, may repeat every 30–60 minutes) - In severe or unresponsive cases: Consider Vitamin C, transfusion, exchange transfusion, or hyperbaric O₂
🧬 But Wait… Let’s Talk Genetics
Not all cases are acquired. There’s a rare hereditary form of methemoglobinemia due to cytochrome b5 reductase deficiency—typically inherited in an autosomal recessive pattern.
Which brings us to one of the most legendary chapters in rural medical history…
💙 The Blue People of Troublesome Creek
In the early 20th century, a family living in the hills of Kentucky became known for one striking feature:
Their skin was blue. Really blue.
The Fugate family of Troublesome Creek carried a rare recessive gene that caused congenital methemoglobinemia. Generations of intermarriage in the isolated region led to several descendants with visibly blue-tinged skin.
A local hematologist eventually diagnosed and treated them with—yes—methylene blue, which restored normal skin color within hours.
The story of the Fugates is now part of both medical lore and Appalachian folklore, reminding us that even rare physiology can paint a vivid picture—literally.

🩺 Final Thought
If a baby looks blue, don’t stop at the lungs and heart.
Check the blood.
Because sometimes, cyanosis is just the tip of the (chocolate-colored) iceberg.
Read more about the Fugates here.
Read the original journal article on the Fugates here.

Dr. Joshua Belfer, MD, is a Pediatric Emergency Medicine physician at the Children’s Hospital of Philadelphia, and is the Founder and Editor-in-Chief of HipPEMcrates. He can be reached at HipPEMcrates@gmail.com.


